WARNING: This story contains details that some readers may find distressing.
Dr Raymond Kipakapu’s first encounter with a survivor of sorcery accusation related violence (SARV) was a profound challenge, not just medically, but personally.
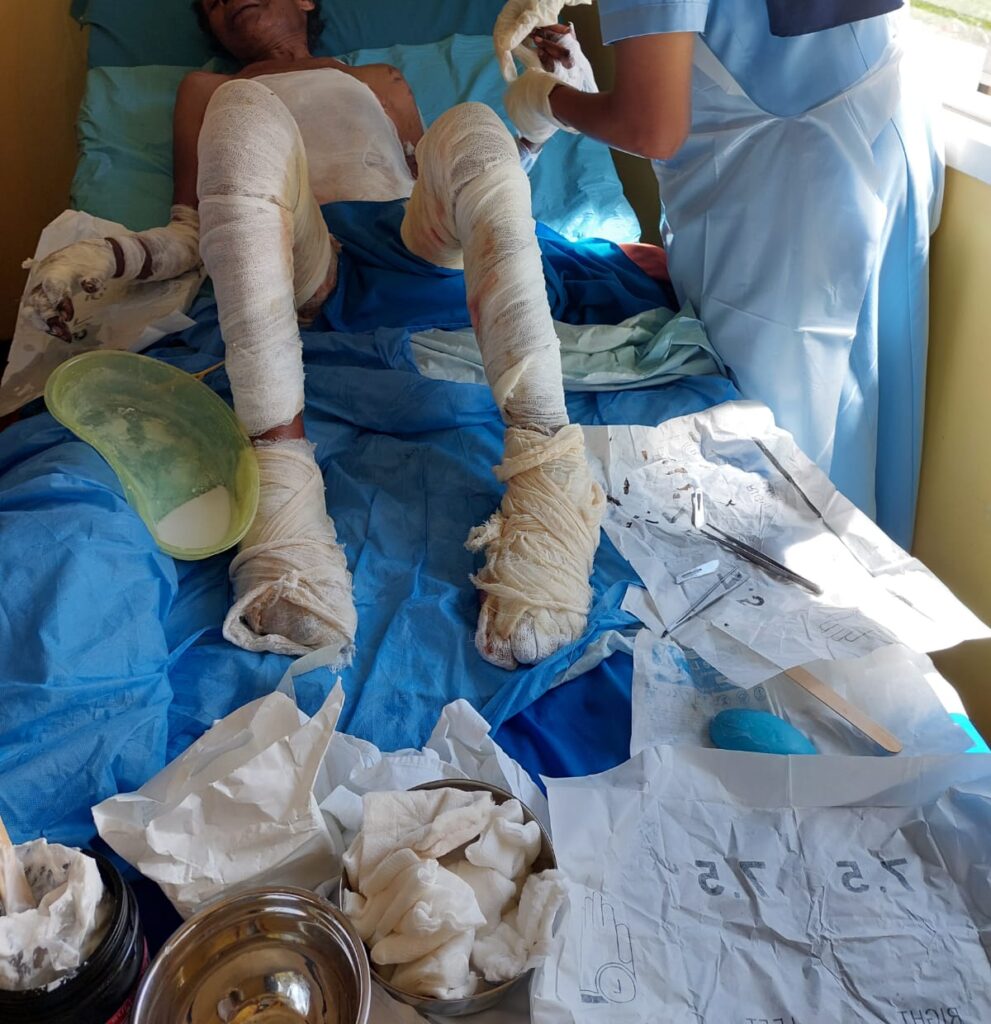
Fresh out of medical school, he was confronted with an elderly woman rushed to the hospital with severe burns to her legs, arms, and other parts of her body. Her daughter, a woman in her 40s, had also been injured. Both had been held captive and tortured for days before their rescue.
The severity of their injuries was harrowing, but for the young doctor, the case presented a deeper, more internal struggle.
“I have to be honest, I was a bit scared,” Dr Kipakapu said, reflecting on the moment.
Growing up in Papua New Guinea, he was immersed in cultural traditions and protocols. The late-night stories of shapeshifters and malevolent spirits, often depicted as elderly women, echoed in his mind as he entered the patients’ room.
“It was difficult to detach himself from strong cultural beliefs and focus on treating his patients as a man of science,” he recalled.
He credits the guidance of his more experienced team for helping him navigate the complex situation.
“I had to observe how my team reacted,” he said. “With a lot of case management in the past, the team was confident. Without any prejudice, they approached the patients. So, I just followed my team’s lead.”
Dr Kipakapu’s experience sheds light on a broader issue in Papua New Guinea, where irrational fears of sorcery can burden professionals across many fields, including medicine.
From Port Moresby’s bustle to the rural frontline
Dr Kipakapu began his medical career in 2018 at the Port Moresby General Hospital. The demanding urban environment served as a crucible, honing his skills in emergency care and surgery within the nation’s overstretched healthcare system. However, a subsequent move to rural practice, serving in Tinsley in the Western Highlands and later at the Yambu Health Center in Enga Province, reshaped his perspective on medical care.
In these remote settings, far from the resources of the capital, he was forced to adapt, treating everything from malaria to maternal emergencies with limited equipment. It was in Yambu that his focus shifted dramatically towards the horrific injuries inflicted upon those accused of sorcery.

Now seconded from the Enga Provincial Health Authority to the Catholic Health Services, Dr Kipakapu is one of the few doctors in the country specialising in the treatment of SARV survivors.
“Many of the patients come with first, second and third-degree burns,” he said.
“We’ve seen cases of people who have been tortured for days… two days, three days… People keep them outside, hang them up with wires and keep torturing them until they get a confession or admission of guilt.”
In 2024 alone, Dr Kipakapu and his team have treated 20 SARV cases in Enga Province.
A nationwide crisis
The violence in Enga represents a fraction of a deep-seated national problem.
Over the past decade, men, women, and children have fallen victim to brutal attacks fuelled by sorcery accusations. Disturbingly, many of these incidents are filmed and shared on social media, where comments often reveal a widespread ignorance and, in some cases, support for the violence.
High-profile cases have occasionally pierced the public consciousness. In 2017, swift police action in Lae saved a woman from torture after she was accused of sorcery following her husband’s death from an unrelated illness. Days later, another woman was killed and her body dumped in the same area.
The scale of the problem is immense. A multi-year study in Enga Province documented 198 incidents of SARV. According to the Papua New Guinea Tribal Foundation, which works to rescue victims, over 6,000 cases were recorded across the country between 2016 and 2021.
These statistics underscore the urgent need for effective interventions to combat the devastating impact of SARV on individuals and communities.
The invisible wounds of trauma
Addressing sorcery accusation related violence requires confronting a complex web of cultural beliefs. For Dr Kipakapu, medical training alone is insufficient to tackle the root causes.
“In Enga, when you speak, you have to speak from a position of authority,” he said.
“You need to have walked the path in order to give credence to your words. I am not a pastor. So, when I speak, I can only do so from a medical perspective.”
Beyond the visible scars, Dr Kipakapu is working to draw attention to the unseen consequences of this violence, such as post-traumatic stress disorder (PTSD) and the generational trauma that affects the children of survivors.
In cultures where retribution is common, the cycle of violence rarely ends with the initial accusation, leaving a lasting legacy of fear and suffering.






